Around 9 weeks ago, I wrote my first article on the COVID crisis titled “Navigating Through The “Coronavirus-Panic”: 8 Inconvenient Facts To Consider”.
My goal with this intentionally-prudent article was to put forward a very balanced view of the situation, and make readers aware of several areas where media coverage didn’t reflect the reality; i.e. where the ‘other side’ of the story wasn’t being told (ex: the slew of international experts who didn’t agree that COVID is a particularly dangerous virus).
Weeks later, the conclusions I had previously come to have only been reinforced, and I must admit I’ve been really tempted to write a massive follow-up “I told you so” article. My ego begged for it.
After re-writing this intro around 7 times (and counting), I’ve come to realize that the average person’s fear and despair tank is already overflowing — and that the last thing that’s needed in this current climate is more negativity.
In this second and final 3-part COVID article, I’ll therefore focus on the good news: We’re going to be fine, we can stop panicking, and the worst of this crisis is already far behind us.
“How dare you give us good news? More than 300,000 people (and counting) have already died from this devastating virus, and the second wave will be even worse!” If that’s how you currently feel about people who try to argue that the crisis is nearly over, then I hope this article will at least be a partial cure to your anxiety, and help you rid yourself of the “corona-panic” that billions of people around the world are still struck in.
To make the argument that “we’re going to be fine”, that the COVID crisis is basically over, and that — yes I’m going to go there — we can and should go back to “normal”, I’ll dive deep in 5 different facts that have been mostly ignored and even censored in the media coverage we’ve seen in the last months.
Table of Contents
Fact #1: We Can Stop Fearing New Daily Cases of COVID, Since That Figure Is Basically Meaningless
1.1 Reality Check: The Number of COVID Cases Is Actually Meaningless
1.2 Scary Outbreaks, Or Just More Testing?
1.3 The Validity of RT-PCR Tests Is Highly Questionable
1.4 The Latest COVID-Craze: Thousands of Untested Cases Now Considered “Confirmed”
Ending The “Corona-Panic”: What To Do About COVID Cases
2.2 It’s Unlikely That COVID Really Causes Every Symptom Under The Sun
Ending The “Corona-Panic”: What To Do About COVID Symptoms
Part 2: Read It Here
Part 3: Read It Here
Fact #1: We Can Stop Fearing New Daily Cases of COVID, Since That Figure Is Basically Meaningless
The same journalistic or political treatment we’ve seen for COVID-19 would cause just as much fear if we applied it to any regular flu season. [my translation, source here]
– Didier Raoult, MD, PhD, rated #1 expert worldwide in Communicable Diseases, author of 2,300 indexed publications
Nothing has caused more panic worldwide than the daily reporting of new cases of COVID in the media.
At the very beginning of this saga, the Johns Hopkins “big-red-dotted” COVID map/tracker was already receiving 1 billion fear-inducing, nerve-wrecking page refreshes every single day.
Unsurprisingly, a US survey found out that 13% of all Americans — that’s 42,436,000 people — believed they had COVID on March 16th. On that date, however, we had only identified 4,226 cases of COVID, and seen 88 people die from it.
Very rapidly, the panic got out of hand. Everyone who coughed had COVID. Everyone who felt sick had COVID. And everyone who died probably died from COVID. But the reality — the hard numbers — tell a very different story.
1.1 Reality Check: The Number of COVID Cases Is Actually Meaningless
At the time of this writing (May 20th), the now (in)famous Johns Hopkins COVID-19 Map shows nearly 5 million confirmed cases of COVID around the world.
Even if we assume that all these “confirmed cases” are indeed “confirmed”, and don’t even argue about the validity of the RT-PCR test that was used to confirm the presence of COVID, the total number of infections is a meaningless number by itself.
A case of COVID simply means that the SARS-CoV-2 virus, or at least the 100 nucleotides that are thought to be specific to SARS-CoV-2, has been detected in a person’s saliva, respiratory tract or stool. (more details here)
A case of COVID does not equal a person with symptoms. It does not equal a person who has been or currently is hospitalized. It does not equal a person who has died or will necessarily die from COVID.
The data we have on COVID is far from being set in stone (it gets more and more precise as time goes by), but what we know so far is that:
1) At least 50% of “test-positive” people of all age groups are asymptomatic. They have or had COVID, but never felt anything (see Fact #2 for more details).
2) The hospitalization rate from COVID (how many people get COVID and end up going to the hospital) in the US will likely be similar to a mild flu season.
3) The overall IFR (Infection Fatality Rate — what fraction of people who get the virus actually die from it, including the asymptomatic and undiagnosed folks) for COVID will likely end up being somewhere in the range of 0.1-0.4%, which is similar or slightly higher than a harsh flu season (see Fact #4 for more details in part 2 of this article).
1.2 Scary Outbreaks, Or Just More Testing?
The math is pretty simple, but has been mostly ignored in the media.
The more you test, the more COVID cases you find, and especially in early stages of a new pandemic — since testing is often concentrated in symptomatic people.
Testing out the entire population on the exact same day to get a perfect portrait of how widely the virus has spread is basically impossible, so the next best thing that can be done is testing as much as possible (often focusing on risk groups and medical personnel) all while keeping a close eye on what’s called the “COVID-positive test rate”. This refers to what percentage of all tests come out positive.
If you test 100 people and 5 of them are positive with COVID, this equals a COVID-positive test rate of 5%. If the next week you find out that 6 out of 100 people who get tested are positive, and the next it goes up to 8 out of 100 people — the upwards trend could be indicative that the virus is starting to spread more widely in the population.
If, on the other hand, you see that number go down gradually, that’s a good sign that the virus spread has either slowed or is dying down.
There’s a tricky part here — an inconvenient fact that caused a lot of panic in the media: If you increase your testing capacity (how many tests you perform on a daily basis), the number of COVID cases you find will logically go up by a proportionate amount (should the COVID-positive test rate stay constant).
Here’s what I mean. Let’s take my previous example, and imagine that we are testing 100 people per day, and finding out that 5 of them have COVID. That’s a COVID-positive test rate of 5%. So far so good, and the media report that once again, we’ve identified 5 new COVID cases today.
Eventually, health authorities decide to triple how many tests they perform each day, in order to quickly identify “outbreaks” and act accordingly, and get a more precise idea of who is infected, and who is not. The number of tests goes from 100 to 300 per day. From that day forward, health authorities now report that they’re finding 15 new cases of COVID cases every single day.
15 new COVID cases? That’s a 300% increase. Looks like we’re seeing a huge outbreak. But are we really? What has increased is simply the number of tests that are performed every day. In reality, the overall COVID-positive test rate is still 5%.
Enough with the examples… here’s the problem. Several researchers have identified that so far during the COVID crisis, the COVID-positive test rate has been fairly stable, oscillating between 10 and 20% — an inconvenient fact that speaks against the idea that the virus has been spreading exponentially.
A) Biophysicist Felix Scholkmann
Scholkmann has graphically organized the COVID-positive test rates of several countries (Germany, USA, Japan, Switzerland, UK). The data (early March to April 24th) clearly shows that the rate doesn’t go up, which “speaks against a current viral epidemic” (SPR)

Image credit: Felix Scholkmann

US: Total number of positives and negative tests vs. rate of positive tests (April 2). Image credit: Felix Scholkmann
B) Data from Norway
This data analyzed by a PhD in environmental toxicology dates back from March, but clearly shows that “the rate of test-positives does not increase – as would be expected in the case of an epidemic [emphasis mine] – but fluctuates in the normal range for coronaviruses between 2 and 10%.” (Via SPG)

C) German researcher Richard Capek — March data from NYC
Capek has demonstrated the exact same phenomenon. In March in New York City, while the American media and government were still pushing the idea that the virus was spreading in an exponential manner, the COVID-positive test rates increased only slightly, fluctuating around 10 to 15%.

Image credit: Richard Capek. Capek explains, about this graphic: “The blue curve shows the development of the infected portion of the accumulated values, the orange curve the daily values. You can see a leading increase in the proportion of infected people (cumulative) since March 16, 2020, rising from approx. 10% to 15%. It now reaches a value of 15%.”
D) Professor Christopher Kuhbandner — data from Italy and Germany
In a recent article, Prof. Kuhbandner argues that “the thesis of the epidemic spread of the coronavirus is based on a statistical fallacy.”
Analyzing the official data from Italy and Germany, Kuhbandner concluded that:
The reported numbers of new infections very dramatically overestimate the true spread of the coronavirus. The observed rapid increase in new infections is almost entirely due to the fact that the number of tests has increased rapidly over time. [emphasis mine] So, at least according to the reported numbers, there has never really been an exponential spread of the coronavirus.

Image credit: Prof. Christof Kuhbandner. In red: “Artificial increase in new infections due to the increasing number of tests”. In green: “Estimated true increase in new infections.”
Referring to the graphic above, he explains:
As you can see, the reported numbers of new infections dramatically overestimate the real increase. The reported numbers give the impression that the number of new infections has increased by up to 27 times, although in reality the number of new infections has only increased by a maximum of 4 times. Furthermore, it can be seen that the number of daily new infections actually begins to decrease earlier than the reported numbers of new infections appear to be. [emphasis mine]
To put these figures in context, normally during flu pandemics you would expect the flu-positive test rate to go from around zero before the flu season, all the way up to 60-80%, and then all the way down to near zero. Here’s an example of a typical flu season in Germany in 2017 (data from the German Robert Koch Institute):
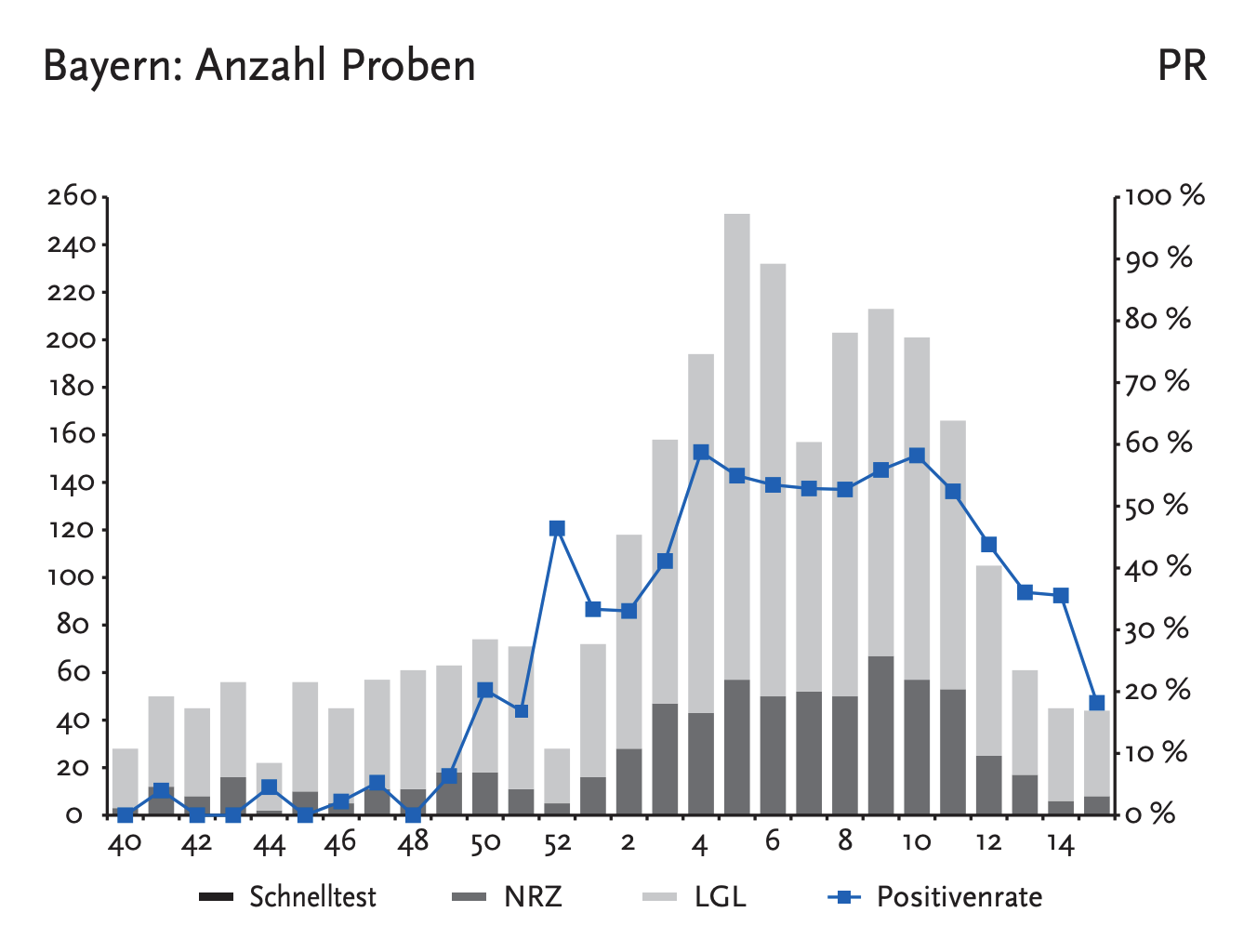
2017-2018 flu season in the German State of Bavaria. Notice the flu-positive test rates going up to 60% during week 4 of 2018, and eventually falling down below 20% on week 15. Image credit: Robert Koch Institute
And here’s a similar curve we’ve seen so far during this 2019-2020 flu season in the United States:

Source: CDC Weekly U.S. Influenza Surveillance Report – October 1st 2019 to April 25, 2020.
What does this all mean? These findings support the idea that a large fraction of the population already has COVID, and that as long as we keep testing, we’ll keep finding new cases of COVID. This also means that we should not panic if the number of new daily cases goes up as we increase how many tests are done every day.
Do we have indications that COVID has been spreading much more widely than we previously thought? You bet.
- Recent autopsy findings in the US confirm that the first person to (allegedly) die from COVID was a 57-year old woman from Santa Clara County, California, on February 6th — much sooner than what had been previously considered the first COVID death on February 29th.
- A recent serological study from Stanford also found that the prevalence of COVID in Santa Clara County is “50 to 85 times more common than official figures indicated”. Dozens of similar studies have come to similar conclusions in many countries — each indicating that COVID has already spread widely. I’ll list them a bit later in this article.
- New indications from France show that the “patient zero” in this country might have been on November 16th, months before the official timeline.
1.3 The Validity of RT-PCR Tests Is Highly Questionable
I’ve addressed these problems in length in my last article — but in the last few weeks I’ve seen several additional indications that the tests we’re using to detect COVID are extremely prone to error. Here are a few key examples:
A) The RT-PCR test shouldn’t be used to diagnose a disease in the first place.
At least that’s what Kary Mullis, the scientist who happened to invent the RT-PCR test and received a Nobel prize because of it, argues:
‘Quantitative PCR is an oxymoron.’ PCR is intended to identify substances qualitatively, but by its very nature is unsuited for estimating numbers. Although there is a common misimpression that the viral-load tests actually count the number of viruses in the blood, these tests cannot detect free, infectious viruses at all; they can only detect proteins that are believed, in some cases wrongly, to be unique to HIV. The tests can detect genetic sequences of viruses, but not viruses themselves. [emphasis mine]
To be clear: The RT-PCR test does not and cannot detect the SARS-CoV-2 virus itself, but a specific RNA section that is thought to be specific to SARS-CoV-2. It does not and cannot assess the viral load — how much virus is in someone’s blood. It does not and cannot demonstrate that the presence of a virus has caused a certain disease, or certain symptoms. It does not and cannot be used alone to diagnose any disease.
As pointed out by the nonprofit organization Swiss Propaganda Research, American diagnostic manufacturer Creative Diagnostics even specifies that “the detection result of this [COVID-19 test] is only for clinical reference, and it should not be used as the only evidence for clinical diagnosis and treatment.”
This flies in the face of the WHO’s definition of what a “confirmed case” of COVID is, which they define as “a person with laboratory confirmation of COVID-19 infection, irrespective of clinical signs and symptoms.” [emphasis mine]
In other words, the WHO — and governments worldwide who follow their lead — are perfectly comfortable with the idea of using a test which should technically never be used for diagnostic purposes… to diagnose COVID.
B) Dozens of different RT-PCR tests are being used, each with slightly different definitions of what constitutes a “positive case” of COVID.
Canadian independent researcher of infectious disease models David Crowe has analyzed the instruction manuals of 33 different PCR tests approved by the US Food and Drug Administration (FDA). What he found was so confusing that he ended up poetically describing them as a “Potpourri of tests”.
This gets technical, but some clear examples of discrepancies include:
- Most tests use a different number of PCR cycles to distinguish what is considered a “positive” from a “negative” result.
One manufacturer each recommended 30 cycles, 31, 35, 36, 37, 38, and 39. 40 was the most popular, chosen by 12 manufacturers, and two recommended 43 and 45. The MIQE (Minimum Information for Publication of Quantitative RT-PCR Experiments) guidelines for operation and reporting of RT-PCR states that the use of 40 or more cycles is unwise.
Crowe recently interviewed Stephen Bustin, a professor at Anglia Ruskin University in the UK — who’s arguably the world’s top expert on quality control of RT-PCR. Bustin said that he doesn’t think that more than 35 PCR cycles should ever be used. Crowe concluded that “the majority of COVID-19 RT-PCR tests approved by the FDA may be pushing RT-PCR to its limits or beyond”.
- The amount of DNA extracted from a patient’s sample can vary widely.
PCR tests can only be performed on DNA, which means that the RNA extracted from a patient’s saliva, respiratory tract tissue or stools needs to be converted into cDNA (complementary DNA) through a process that is unfortunately “quite inefficient”.
Stephen Bustin admitted that “the amount of DNA obtained [from this conversion] can vary widely, easily by a factor of 10.”
Crowe grudgingly concludes that:
Since the PCR cycle number is a measure of the amount of material obtained, different efficiencies essentially invalidate the simple use of the PCR cycle number. Two different test setups in two different labs, that both use the PCR cycle number 35 as a cutoff, may actually have the cutoff between negative and positive at wildly different places. [emphasis mine]
- Most tests have a different definition of what they’re actually looking for.
As I mentioned previously, the RT-PCR test cannot identify the SARS-CoV-2 virus itself, but can identify the presence of the tiny fraction of its genetic sequence that is currently thought to be specific to SARS-CoV-2, and different from other coronaviruses.
Crowe explains that the definition of what constitutes this “specific” genetic sequence varies widely from test to test:
A test developed by Charité Berlin (not on the FDA list) looks for the RdRp and E genes, which amount to 213 base pairs out of about 30,000 for the entire genome, or less than one percent.
On the FDA list, the tests reference the E, N and S genes and portions of the ORF (Open Reading Frame). What is most important to know is not what the function of these RNA segments is, but simply that the tests are looking for very different things. [emphasis mine] It is as if we went looking for leopards with one person using spots as the guide, another the claws, another the teeth and another the eyes.
You know where I’m going with this, and yes, it does get worse. Read on:
Worse than differences in what they are looking for is the way of defining whether they have found it. [emphasis mine] Some tests look for one portion that must be present for the test to be declared positive. Others look for two portions and both must be positive, while others only require one of the two to be positive. Some tests look for three portions, and generally only require two to be detected, although one test requires all three.
If your head is buzzing already with all the technical jargon, simply understand that this means all 33 FDA-approved tests have widely ranging definitions of what constitutes a “confirmed case” of COVID.
C) The RT-PCR tests can react with other coronaviruses, including coronaviruses commonly found in other animals.
On April 22nd, the CDC announced that COVID had been identified in two cats in New York City. The virus had been found in zoo tigers, dogs, and other cats in Belgium and China.
While a lot of people feared that these new findings meant that the virus could now spread through household pets, the CDC stressed that “at this time, there is no evidence that animals play a significant role in spreading the virus that causes COVID-19” and that “based on the limited information available to date, the risk of animals spreading COVID-19 to people is considered to be low.”
According to Dr. Wolfgang Wodarg, who’s been a vocal critic against our reaction to COVID (he has coined the term “corona-panic” in my opinion) in the last several months, the fact that COVID is found in animals is a definite proof that COVID tests are not specific enough, and are wrongly flagging other coronaviruses as “COVID-19”.

On April 22nd 2020, the CDC announced that COVID had been identified in two domestic cats in New York City.
Image credit: NBC News
As early as mid-February 2020, I had recommended testing the [COVID-19] test for its informative value [by] using a very simple method: “Test your cat!”
If the test also reacts positively in animals, then it is not specific enough for the SARS-CoV-2 virus. [The test] apparently also gives false positives for other SARS viruses […]. Apart from that, a PCR test is by no means a sufficient basis for a medical diagnosis.
Now that two domestic cats are positive after tigers, dogs and lions in New York, those responsible and their “fact checkers” have to decide: Do they want to continue listening to the Drosten fairy tales and ruin the country, or do they finally see that they are getting involved in contradictions, getting more and more mistaken and making a fool of yourself? [Google translation, source here. Note: Drosten is a German virologist who was key player in the development of these COVID test kits back in January]
This is not the first and certainly not the last indication that COVID tests might give a false positive result when reacting with other coronaviruses.
In the original paper published on January 23rd by Drosten et al. (which has pretty much influenced how all COVID tests worldwide have been developed), scientists admitted that “virus-positive detection of these phylogenetic outliers within the SARS-related CoV clade suggests that all Asian viruses are likely to be detected.” In other words, there’s a chance that COVID tests might give a positive result when someone is infected with other viruses of the SARS family.
Wodarg boldly concludes: “If we didn’t have the [COVID] test, we wouldn’t notice a ‘pandemic’!”
Recent news from Tanazania show that at least some politicians are as worried as Wodarg that this pandemic is really a pandemic of testing. In a bold and hilarious move, Tanzania President Magufuli (who had doubts about the validity of COVID tests) decided to anonymously send his lab technicians a variety of samples taken from fruits or animals, labelling them with the name of fictive patients. Here’s what he found:
On Sunday President Magufuli, who has consistently downplayed the effect of the virus, shocked the world when he said animals, fruits and vehicle oil had been secretly tested at the laboratory. Now, take a look at some of the specific things he said had been tested. A papaya, a quail and a goat. All of them he says had been found to be positive for COVID-19. [emphasis mine]
Magufuli cast doubt on the credibility of laboratory equipment and technicians and questioned official data on the pandemic. He called for an investigation into what he suspected to be a ‘dirty game’ in the laboratory. Where the kits had been imported from though, he would not say. So, the lab director here Nyambura Moremi has been fired. And a 10-person committee has been formed to investigate the laboratory’s operations, including its process of collecting and testing samples. Presently, that is, as of May 5th, Tanzania has about 480 Covid-19 cases including 16 deaths.
D) False positives, false negatives, and more confusion.
In an in-depth article series addressing the many holes in the COVID narrative, author and independent researcher Iain Davis addressed the problem of COVID tests in length.
As he puts it perfectly:
It seems scientific claims that C19 numbers are underestimated are fine, claims they are overestimated are not. [emphasis mine] Either way, whether false negative or false positive, there is plenty of evidence to question the reliability of the RT-PCR test for diagnosing COVID 19.
Quick refresher: a “false positive” refers to a test giving a positive result, when in reality the result is negative. Ex: You’re told you’re infected with COVID, when in reality you’re not. Too many false positives can lead to an overestimation of how widely COVID has spread, and an overestimation of how big of a problem it might constitute.
A “false negative” is the exact opposite — and refers to a test giving a negative result, when in reality the result is positive. Ex: You’re told you’re not infected with COVID and can happily move on with your life, when in reality you do have COVID. Too many false negatives mean that a lot of people who think they are COVID-free might spread COVID to other people.
In my previous article I had mentioned a Chinese study which did show that the COVID tests had up to an 80% false positive rate — but the study has now been retracted, over “political reasons”. Who knows what’s really up with that study… but it’s definitely not the only one which found that the tests are prone to a lot of errors.
This large error margin can lead to devastating problems, including people getting treated for a disease they don’t have (consider that intubation has a tremendously high death rate — more on this later), medical staff being quarantined because of a virus they don’t even have, or even to transmission of COVID to risk groups, like in nursing homes.
One example which comes to mind is how one Montreal-based nurse has been repeatedly testing positive nearly a month after she was infected with COVID.
As I mentioned in my last article, 14% of ‘recovered’ patients in China test positive again for SARS-CoV-2. I’ve since learned that it’s not completely impossible to become reinfected with a virus right after you’ve had it, but the other possibility is that these people never actually had COVID. They were false positives.
Recent findings from South Korea confirm this is probably the case: the strong false positive rates are probably responsible for what we perceive as “reinfections”.
More than 260 COVID-19 patients in South Korea tested positive for the coronavirus after having recovered, raising alarm that the virus might be capable of “reactivating” or infecting people more than once. But infectious disease experts now say both are unlikely. [emphasis mine]
Rather, the method used to detect the coronavirus, called polymerase chain reaction (PCR), cannot distinguish between genetic material (RNA or DNA) from infectious virus and the ‘dead’ virus fragments that can linger in the body long after a person recovers, Dr. Oh Myoung-don, a Seoul National University Hospital doctor, said at a news briefing Thursday (April 30), according to The Korea Herald.
For more research on the topic, watch this analysis by Dr. John Campbell.
1.4 The Latest COVID-Craze: Thousands of Untested Cases Now Considered “Confirmed”
One of the various eyebrow-raising developments during this COVID crisis happened when several governments throughout the world took decisions that led to an artificial inflation of the number of COVID “confirmed cases”.
Some decision makers argued that changing what is defined as a “confirmed case” to include cases that were untested but were “probable” were done to avoid dangerously underestimating the real danger that COVID represents (especially since we cannot possibly test everyone). The other side of this coin is that this also can lead to a vast overestimation of the risks.
I cannot find who said this (let me know if you find who this needs to be attributed to!), but someone perfectly summed up in a recent article that “politicians will never be blamed for doing too much, but will definitely be blamed for not doing enough”. This is at the core of the case-inflation problem.
While the world was busy watching apocalyptic media reports coming out of the COVID outbreak in New York City, the reality is that the number of total detected COVID cases was actually going down by an average of 0.94% every single day — definite proof that the worst part of the crisis was already behind us.

% change in Daily US increase rate in cases (7-day rolling average) based on the Johns Hopkins data.
Image credit: Walt Lundy, Balance Nation Facebook group.
This downward trend started reversing around April 14th, when New York City officials decided to include “probable” cases and deaths to the official figures.
A look at a graph of new daily cases (based on the Johns Hopkins tracker) clearly demonstrates how this created the impression that the pandemic was still at its peak (when in reality it was on a rapid downwards trend):

Daily new cases in NYC based on the Johns Hopkins data.
Image credit: Walt Lundy, Balance Nation Facebook group.
Officials explain that “those cases involved people who were presumed to have been infected because of their symptoms and medical history.”
This sounds good in theory, but only holds ground if doctors can easily identify cases of COVID based on symptoms alone.
The reality? They can’t, 96% of the time. White House Coronavirus Response Coordinator Dr. Deborah Birx, reminded everyone on March 14th that: “South Korea saw a 96% or more negative testing rate even though they were testing people with symptoms.” [emphasis mine]
These “probable” cases are not so probable after all. But this didn’t stop several other countries or States from including them in their official case count. For example, the province of Quebec, Canada (where yours truly lives) has “stopped distinguishing between probable and confirmed cases” on March 23rd.
The same loosening of definitions has also been seen for “confirmed COVID deaths” — and I’ll be addressing that later, in Fact #4.
Ending The “Corona-Panic”: What To Do About COVID CasesFor concerned citizens:
For decision makers and the media:
|
Fact #2: Most COVID Cases Are Asymptomatic, And A Large Fraction of “COVID-Symptomatics” Probably Suffer From Something Else
Is there any other virus out there that is this weird in terms of its range of symptoms?
– Carl Zimmer, popular science writer & blogger
A very large fraction of all COVID cases are asymptomatic. You get COVID, and yet you don’t feel anything.
This trend has been seen in Italy (50-75%), on the Diamond Princess cruise ship (50%), in India (69%), China (78%), in Boston, USA — among homeless people (recent serological study — 98% asymptomatic), in New York City — among pregnant women (88%), and among 3,300 inmates across the US (96%) — just to give a few examples.
Giesecke, one of the epidemiologists leading Sweden’s response to COVID, also recently published that “98 to 99 percent of [COVID-positive people] are probably unaware or uncertain of having had the infection.”

On May 6th 2020, only 2% of all active COVID cases reported by Worldometer.com were considered ”serious or critical”.
We should be celebrating those findings. They confirm that COVID is much less deadly than we previously thought (Fact #4), and that, as previously mentioned, the virus has spread much more widely than we previously thought — without causing a major increase in overall mortality (also Fact #4).
When it comes to “symptomatic” cases, the data is a real mess, and there’s a multitude of indications that a lot of symptoms blamed on COVID are in fact caused by other viruses, bacterial infections and other agents.
2.1 Cases Of Other Respiratory Infections (Like The Seasonal Flu) Are Probably Being Slapped With “COVID”
Combine the fact that COVID has already spread much more widely than we previously thought and the fact that the COVID test likely has a very high rate of false positive, and it becomes obvious that a large fraction of all people who get tested for COVID will test positive.
According to Prof. Knut Wittkowski, who headed the department of Biostatistics, Epidemiology & Research Design at the Rockefeller University for 20 years, there are “at least 25% [of all people] in New York City” who have already been infected with COVID. The odds (one out of four) of finding COVID in anyone you test in that city at random are therefore very high.
In the current climate, a lot of people seem to suffer from a major case of confirmation bias, and start panicking the second that someone dies from a “mysterious” or “unexplainable” condition, and happens to also be testing positive for COVID.
Repeat after me: The presence of COVID does not prove that COVID is the one culprit causing symptoms, or that it even was an important factor in their ultimate demise. Correlation does not equal causation.
The media should read the CDC COVID-19 testing kit’s instruction manual a few more times:
- “Positive results are indicative of active infection with 2019-nCoV but do not rule out bacterial infection or co-infection with other viruses. [emphasis mine]
- The agent detected may not be the definite cause of disease.”
Unreasonable memes like “Man Crushed By Steamroller Dies Of Coronavirus” do have a point: If someone clearly dies from a heart attack, and happens to be testing positive for COVID, it does not mean that COVID caused the heart attack. It might have played a role… but maybe it didn’t.
On April 15th, data scientists from the Stanford University School of Medicine published a paper titled “Rates of Co-infection Between SARS-CoV-2 and Other Respiratory Pathogens”, in which they highlighted that 21% of all COVID-positive patients that were tested also had a respiratory co-infection. If these patients die from one of their active respiratory infections… which one caused their demise?
While we do need more studies before we can safely extrapolate this data to the entire population, the fact remains that these co-infections might create a lot of confusion in our assessment of who is actually sick because of COVID, and who actually dies from COVID.
2.2 It’s Unlikely That COVID Really Causes Every Symptom Under The Sun
It looks like every other day there’s a new symptom or condition that’s being blamed on COVID. As reported by The Intelligencer:
The clinical shape of the disease, long presumed to be a relatively predictable respiratory infection, is getting less clear by the week. Lately, it seems, by the day. As Carl Zimmer, probably the country’s most respected science journalist, asked virologists in a tweet last week, ‘is there any other virus out there that is this weird in terms of its range of symptoms?’
Science mag reported that according to the experience of clinicians treating COVID patients worldwide, the virus can cause “a ferocious rampage through the body, from brain to toes”.
Both of these articles did make a good point: There’s still a lot we don’t know about COVID. I’ll give you that.
But what stunned me is that both articles overlooked two very plausible reasons that COVID would be able to cause such a bizarre laundry list of symptoms:
A) Medical interventions used to treat COVID might be responsible for some of these symptoms, and some of the COVID deaths.
We know that intubation probably isn’t the way to go, given that out of 5,700 patients hospitalized in the NYC area, 88% of those put on ventilators died (that death rate went up to 97.2% for patients over 65 years of age). Normally, you would expect around 40 to 50% of patients with severe respiratory distress to die while on ventilators.
This abnormally high death rate following invasive intubation has led to a slew of new studies which recommend to minimize their use. Mechanical ventilation is a serious medical intervention which can lead to ventilator-induced lung injury and many other complications, including death.
A 2017 study, published by a research team at the Johns Hopkins Armstrong Institute of Patient Safety and Quality, describes some of these risks:
A ventilator can provide much-needed assistance to patients with their breathing. Being on a ventilator, however, also comes with risks and can lead to complications, or ventilator-associated events, such as blood clots, lung damage or ventilator-associated pneumonia — believed to be one of the most common and deadly hospital-acquired infections in the ICU. [emphasis mine]
To be clear: I’m not here to put blame on how the medical system dealt with the COVID crisis, and it’s likely that invasive ventilation looked like the right intervention to use at the time. But now that new information has come out, it’s critical to revise medical protocols as soon as possible.
Lately, a team of doctors at UC Chicago have witnessed “truly remarkable” results using ventilator alternatives to treat COVID patients under respiratory distress.
They used “high-flow nasal cannulas” (HFNCs) instead of invasive intubation on dozens of patients, and they “all fared extremely well, and only one of them required intubation after 10 days.” [emphasis mine]
Some of the symptoms we’re seeing might also be due to the use of several drugs during the treatment of COVID:
- Corticosteroids: might suppress the immune system, increase overall mortality and increase the the rate of secondary bacterial or fungal infections (source)
- Very common classes of drugs: “several widely used medicines, such as antipsychotics and antidepressants, opioid analgesics, anticholinergic drugs, gabapentinoids, proton pump inhibitors, and inhaled corticosteroids can increase the risk of pneumonia by 1.2 to 2.7 times. […] Elderly patients are particularly likely to receive one or more of these drugs.” (source)
- Antimalarial drugs such as chloroquine and hydroxychloroquine: these might show some promise, but can lead to hemolytic crisis (includes possible acute and severe anemia, kidney damage, blood clots) for people with favism, a deficiency of G6PD enzyme. About 400 million people worldwide fall in this category, and this might be one of the reasons why certain subsets of the population like African-American men seem to die more frequently from COVID. (source)
B) Quite obviously, what is being put under the “COVID” umbrella might actually be a slew of different conditions.
Considering that doctors fail to recognize COVID 96% of the time based on symptoms alone, and that COVID tests are very questionable, several of the symptoms that are blamed on COVID might be due to a large list of other conditions.
Several conditions seen in children have been recently linked to COVID, including:
- Bizarre cases of toxic shock and “atypical Kawasaki disease” (the WHO and the UK Kawasaki Disease Foundation now both said to stop making that link)
- Heart attacks in young COVID patients (in their 30s and 40s)
What is important when coming across these news is looking at how many people have actually been diagnosed with this condition, and whether these conditions existed before COVID was in circulation.
For example, in the case of heart attacks in young adults and children, these have been an increasing problem for years. The Cleveland Clinic recently explained that “although Americans are suffering fewer heart attacks as a whole, the rate of heart attacks for people under 40 is increasing.” This is an increasingly concerning problem in young adults in their 20s, and even in teenagers.
So far, these are nothing more than anecdotes reported by the media still struck by a solid case of “corona-panic”. These reports simply do not reflect what has been observed by scientists worldwide based on more than 5M of “confirmed” cases of COVID: Children actually face a lower risk of dying from COVID than from the seasonal flu. (more on this in Fact #3)







11 Responses
From the beggining I read a couple of articles thst made me question just how ‘deadly’ the Covid19 is,…and made me think it’s probably not much more deadly than the seasonal flu(the articles questioned the reliability of tests,as u have). However, as i am in the ‘high risk’ group, it didn’t give me, personally,much reassurance. Also, as time has gone by, and the number of daily deaths by Corona were increasing, it was even more worrying( i rarely look at the increase in total number of infections, cos like u say, it isn’t a valid way of assessing things. So i usually just look at the daily deaths).
I think u bring up alot of valid points…
However, here in the U.K., the total number of ‘excess deaths’, (meaning more than what would usually be expected in the same period of time, as an average deaths), has been around 50,000. Around 30,000(can’t remember exact figure..might be 33,000) have been attributed to Covid 19 deaths, and the rest were ‘indirecly’ caused(eg: people avoiding going to hospital for other health conditions, cos of fear of contracting the virus whilst there.). U do not appear to mention this vital ‘statistic’, in this article,…the ‘excess deaths’. Can u please explain why that is?
Also, if u were in the ‘high risk’ group, u might have had a slightly different view of things, shall we say. When u say ‘aslong as we protect the high risk group’, when lock-down is lifted, there won’t be much to worry about, …I am thinking that the ‘high risk ‘ group is probably quite a high percentage of the population…and they deserve to be protected better. That’s my view, at the end of the day…I wouldn’t be agreeing with lock-downs,and social-distancing, being removed completely. Also, another point u seem to fail to acknowledge, is that if there hadn’t been lock-downs….the ‘excess death’s would have been exponentially higher.
Am I missing something here..?
Last point I’d like to make, is that the potential serious effects that Covid19, has on some people’s health, is far worse than the common flu (eg:for one thing, Covid attaches to receptors in the heart, causing serious problems there.).. It seems to have some horrendous effects, at times. Tho I agree with u, that some of the damage done to patients was through the actual med interventions( what u say about using nasal-tubing, instead of throat,being far more safe, and effective, is v interesting…and is important info that needs to be spread.)
Part 2 and 3 will address death rates, death reporting and whether lockdowns have saved lives or not. There’s no real indication that COVID is more deadly than a lot of common coronaviruses and other virus including Influenza strains for people in risk groups. It seems to be especially deadly in people who are already at the end of life — as seen in the nursing home crisis. Stay tuned for the rest, everything will make more sense with all 3 parts together.
Thanks for reply. I look forward to the next articles, if they do address the points I made.
Ps. I do respect ur work on Emf, 5G etc and informing people the v real dangers.
Nick, good info. I agree with the perspective presented. Looking forward to parts 2 & 3.
Question: If you were to produce a video wherein you covered in detail all that you’ve covered in this blog, do you think the video would be accepted by mainstream media platforms or would they judge it to be “mis” or “dis” information and block it?
If that video became popular enough, it would quite possibly be banned from YouTube in the current climate.
Nick, I have been following your reporting for several years and appreciate the time and effort you have put in to better inform us. I believe much of what you are reporting about Covid 19 to be plausible and accurate. However, it fails to explain what has happened in New York and Milan, among other “hot spots” , where there was a surge of fatal respiratory illnesses that had not been seen except for perhaps 1918. I believe this is what frightens us the most. If this was not sars 2 Covid 19 virus, some sleuth needs to discover an alternative source.
Julian Simmons
Part 2 and 3 will address these further. A quick explanation is that Italy has seen a mortality rate similar as the rest of the world, however in a much older population. Large fraction of deaths in nursing homes.
Same in NYC — lots of deaths in nursing homes. Their policy to send hospital patients to nursing homes without asking to see a COVID-negative test first was a complete failure. A large fraction of excess deaths are probably due to the lockdown and panic — more on this in Part 3. Deaths are way over-counted in the US, creating unnecessary panic. I think the US will slash their COVID toll by a large margin next year when real retroactive investigation is done.
I’m just waiting for “accident prone” to join the list of symptoms. Also, neuropsychological disorders, which in my highly biased observations I have seen an increase in.
This article provides a certain amount of evidence to support Arthur Firstenberg’s controversial assertion that while there is a SARS-COV2 virus, and it is contagious, the disease itself is not, as he has documented for the case of the 1918 pandemic. At that time, global radio transmissions were first accomplished and the Navy’s ships began using the technology. See his book, The Invisible Rainbow.
At this time, the introduction of 5G is remarkable, but by itself might not produce this effect (the satellite transmissions are a big concern, and I’ve noticed a delay in the arrival of migratory birds, smaller numbers when they do appear, and altered behavior among barn swallows, an earlier migrant who arrived on March 18 in my area, while people have started reporting evidence of strong satellite transmission in April), and even where 5G is not in use, 4G transmissions are said to have increased.
I’ll address it briefly in the part 2, but I have decided to deconstruct why the current narrative of COVID being the apocalypse instead of following the route that Firstenberg has taken — the virus is not contagious. There’s good evidence that the viral theory doesn’t hold ground, but at this moment I’m playing inside the standard view of viruses in order to make a point.
I think that is a wise way to approach this, Nick. Arthur gets rejected out of hand because he rejects the current paradigm entirely without giving his audience a chance to catch up to him. Your reader-friendly approach makes you a real asset to the movement, in my opinion.
BTW, I just ran into an interesting article which is supportive of what you are saying here, pointing out that the response to COVID-19 not only has the overtones of a cult, but it is an actual “cult” phenomenon in the anthropological sense. Against the Corona Panic, Part 7: https://hailtoyou.wordpress.com/2020/05/18/against-the-corona-panic-part-xii-an-anthropological-study-into-the-corona-cult-pro-panic-hardliners-and-the-media-succeeded-in-erecting-a-virus-centered-apocalypse-cult-as-state-religion-and-in/
Worth a glance.
How can anyone still fall for this massive scam-demic hoax? The so called “scientific community” which is 99% corporate Big Pharma/Gates sponsored junk science performed by corrupt “scientists” so far has failed to isolate the alleged Covid-19 virus. So we have no single virus to be tested for in the first place. Then the PCR tests are manipulated/contaminated, not suitable and give false results, then everyone who died the last 3 months is automatically counted as a Covid-death with 99% no autopsy performed – just guesswork. Most patients had at least 1-3 co-morbid factors or were 70+++ of age. Many people died due to deliberately administered false (aka ventilators), over or no medication/treatment. No statistics of other causes of death are being published anymore – everything is CV-19. So CV cured all other diseases from cancer to alcohol/drug abuse, car accidents, old age, etc. Nobody is dying from the common causes of death anymore!
How come so many people cannot see through this and discern it for what it is – a huge worldwide power grab towards establishing a one-world government (plenty of quotes from Kissinger, Gates, Bush, Rockefeller, etc – the usual suspects and fake philantropists). Everything has been meticulously planned for 50 years. This is no conspiracy theory this is a brutal conspiracy. All infos can be found on the World Economic Forum’s website and Event 201 (organized by Kill Gates).
World Economic Forum – WEF
The entire new nasty order is outlined on this website
https://www.weforum.org/platforms/covid-action-platform
Agenda “PLANDEMIC” – 50 Years In The Making – A Must Watch & Share Video!
https://www.youtube.com/watch?v=3hEY8-7jRh4&t=1002s
THE ENTIRE PANDORA’S BOX OF CORONA PLANDEMIC and FAR MUCH MORE! – https://www.weforum.org/